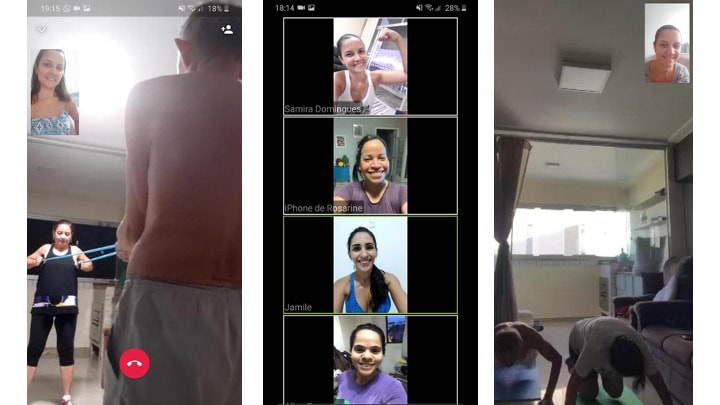
Authors: Prof Samira Bulcão Carvalho Domingues*, Prof Flávia Porto** and Prof Jonas Lírio Gurgel****Master's Degree student, Exercise and Sports Sciences/Institute of Physical Education & Sports/UERJ  Image by Pete Linforth from Pixabay Image by Pete Linforth from Pixabay When faced with the COVID-19 global pandemic, a reduction in the numbers of people circulating is essential. It’s important to know there are differences between social distancing, isolation, quarantine and total lockdown, however, all of these strategies have one goal in common, which is to contain the speed at which the virus spreads and limit the collapse of health systems. In extended social distancing, those establishments considered to be non-essential are closed to avoid the gathering together of people, while in selective social distancing, people belonging to at-risk groups, especially the elderly, are encouraged to stay at home. In isolation, sick people (with suspected or confirmed disease) are separated from the non-sick, whether in a domestic or hospital environment. Quarantine is carried out by those people who have come into contact with or are suspected of having come into contact with the virus and, even if not presenting symptoms, they are isolated from others. When none of these measures work, a total lockdown is declared, like a community quarantine. Although essential, staying at home involves a radical change in the habits of a population, which may harm health in some way. Within the context of epidemiological normality, work, academic and leisure activities require a variety of effort that, taken together, maintain the minimum level of daily physical activity necessary for health, especially for sedentary individuals. An immediate interruption of these activities has a negative impact on the cardiorespiratory and muscle systems, responsible for maintaining functional capacity. This, in turn, is directly related to quality of life and the development of comorbidities. Similarly, and at the same time, physically active individuals are compelled to abruptly interrupt their exercise routines during this period. The damage caused by this halt in training includes losses in muscle strength and mass, aerobic capacity, and joint flexibility and mobility, in addition to alterations in body composition. The change from a physically active to sedentary life can affect important variables for health maintenance, including blood pressure, blood glucose and cholesterol levels. It is therefore advisable to use countermeasure strategies to combat the disuse. One of these is the practice of exercise - known to be the best non-drug health promotion strategy. The American College of Sports Medicine (ACSM) has already taken a position on the importance of staying physically active during isolation. The weekly recommendation for asymptomatic individuals is 150 to 300 minutes of aerobic exercise, plus two strength training sessions. One could, for example, do 5 workouts a week of 30 to 60 minutes, adding muscle strengthening exercises to two of them. The intensity should be moderate, as very light stimuli may not promote benefits, while very high intensities are associated with impaired immunity. Although many people doubt the feasibility and efficiency of home training, the literature shows that results similar to those obtained in traditional gyms can be achieved by using one's own bodyweight as a load. Routines can include exercises based on calisthenics, both in aerobic (stationary running, climbing stairs, jumping jacks) and strength (squats, push-ups, planks) training. Accessible materials can help: elastic bands, skipping ropes, and even household items to increase the workload (water bottles, backpacks with books, bags with groceries).  Training at home, although proven to be easy, affordable and efficient, can be difficult to adhere to on a larger scale. The motivational aspect is certainly one that can suffer, as a large part of the population is sedentary and is not in the habit of exercising; therefore, the absence of commitment to a time and place for training increases the chances of giving up. Another difficulty is in adjusting the intensity and volume of training, especially for individuals with low levels of physical fitness, which can lead to the occurrence of musculoskeletal injuries. Knowing how to do each exercise and how much is essential for the desired positive result, which highlights the importance of professional guidance, because the assumption that "doing anything is better than doing nothing" does not apply to training. Tele-assistance is a reality that is already being used in the health area; and it should also be explored for the prescription of exercise. The options for interaction are varied and can serve the needs of diverse populations. From individual video calls to virtual group meetings, and guidance by messaging apps, the virtual presence of a professional can contribute to both an increase in the motivation of practitioners, and to ensuring that each individual receives the appropriate dose-response exercise.
From Space to COVID-19: what can we learn? We can learn that exercise remains a valid countermeasure to the effects of disuse (as proven by research involving astronauts onboard the International Space Station), that Telehealth can be used in different ways to make practice safer through professional guidance, and that obstacles to training can be similar, especially when there is a drastic change in routine, which alters people's mood. At the present moment, when the home has become a fortress against the virus and the importance of having good health is latent, we hope the practice of guided physical activity at home can be recognised as a way to alleviate the adversities of this very difficult scenario in which the world finds itself. Comments are closed.
|
Welcometo the InnovaSpace Knowledge Station Categories
All
|
UK Office: 88 Tideslea Path, London, SE280LZ
Privacy Policy I Terms & Conditions
© 2024 InnovaSpace, All Rights Reserved



 RSS Feed
RSS Feed