Author: Dr. Paul ZilbermanMedical Doctor, Anaesthetist, Hadassah Medical Center Jerusalem, Israel
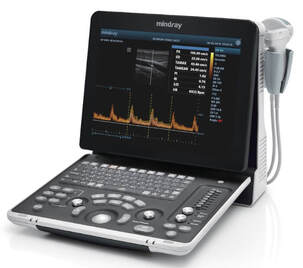
Space is very different, in many aspects. This post does not attempt to address the many changes the human body experiences in space, such as volume modifications in body compartments, fluid shifts, structural configuration in receptor* morphology and, as a consequence, possible variations in pharmacology response, etc. * For the lay reader, a receptor is a special structure on the surface of a cell, for example, that functions as a "receiving point" on which a chemical substance acts in a unique way (like a key – lock mechanism) and a specific reaction is generated (like a muscle contraction) or inhibited (like a cork closing a bottle and blocking the passage of a fluid). These complex structural changes modify many biological reactions, as well as the body’s response to medications. Rather, this post presents some of the technical challenges that an anaesthesiologist may encounter in space. Confined space. On Earth gravity keeps everyone’s feet on the ground. Different pieces of equipment can be repositioned depending on the procedure, machinery can be brought in as needed (XRay scans in orthopaedics, for instance), electric cables can be switched to other convenient wall sockets etc. In a fixed volume space capsule, you don’t have all these possibilities. Everything is measured for maximum volume efficiency. Taking into consideration that anything can and will float if not properly anchored, we can imagine what an “anaesthesia dance” could happen! What equipment? On Earth an anaesthesia workstation is always present in the OR. Depending on its complexity its volume can vary between a medium size fridge to a large double-doored one, just put on its side. You don’t have this amount of deposit in a space cabin, but let’s suppose for one moment that you do - you then need an Anaesthesia Gas Scavenging System (AGSS), which removes the anaesthesia gases that have leaked out or at the end of the procedure. On Earth, these gases are expelled into the atmosphere (there is a lot to talk about this and the greenhouse effects too) and the air currents around any medical facility carry them away. In space you don’t have this. Any gas must be expelled using energy, an active process. Otherwise, the whole cabin will become a big anaesthesia machine with all crew members affected. And, speaking of energy, an anaesthesia workstation is also powered by electricity, which is a limited resource in space, depending on the surface of the solar (or light in general) panels. This energy must be stored and used for other life maintenance systems as well, of which a critical example is the Sabatier reactor that provides oxygen. Regional anaesthesia The simplicity and portability of the necessary equipment makes this type of anesthesia attractive. For peripheral neural blocks all you need is a simple ultrasound machine and dedicated needles. The potential drawbacks are that the technique/s need to be taught on Earth but their “transposition” to space is a bit problematic. If the spinal/epidural anaesthesia is relatively simple to learn, the USG (ultrasound guided) blocks are more challenging. Furthermore, the bodily fluid shift due to the lack of gravity causes many tissues to change their tridimensional appearance, leading to increased difficulty in performing the block.
The cardiovascular responses that accompany spinal/epidural anaesthesia on Earth, in terms of heart rate and blood pressure, are different in space. There may be a lack of reactivity so a certain reduction in blood pressure, for example, might not be compensated. We need to remember that the hostile environment in space, especially radiation, affects not only the human body, but also many sensitive electronic components of medical equipment, leading to possible dysfunction. Monitors can potentially de-calibrate and all the information you receive may become inaccurate. Fluids Preparing and administering a fluid on Earth is routine, however, the lack of gravitation in space poses other challenges: air and fluids do not mix. It is called “lack of buoyancy”. Unless we use special equipment to separate fluids from air nothing can be delivered to the patient. This statement is true also for the anaesthesia vaporiser (a special closed recipient that contains the anaesthesia substance); not only can you not simply fill it the way it would be done on Earth, but even if you could, the anaesthesia liquid that becomes vapour cannot separate from the fluid from which it originates. It just cannot exit the vaporiser. Below is a small example of how liquids behave in space and what happens when a liquid exits a recipient: The same is true for another type of anaesthesia, called TIVA = Total Intra Venous Anaesthesia. This technique uses a dedicated syringe pump that pushes different anaesthesia substances through an intra venous line. It’s a useful technique both in terms of volume and energy expenditure, but again we face the same problems: how to fill the syringe without air bubbles and how to protect the electronics of the syringe pump (in fact a computer in all respects) from the deleterious influences of space radiation!
As you can see, space medicine is a very important topic and many people dream of its future use. Yet, we still have a long way to go! With the advent of intermediary space “stops” and the continuous development of new technologies, every challenge will be solved, sooner or later. Comments are closed.
|
Welcometo the InnovaSpace Knowledge Station Categories
All
|
InnovaSpace Ltd - Registered in England & Wales - No. 11323249
UK Office: 88 Tideslea Path, London, SE280LZ
Privacy Policy I Terms & Conditions
© 2024 InnovaSpace, All Rights Reserved
UK Office: 88 Tideslea Path, London, SE280LZ
Privacy Policy I Terms & Conditions
© 2024 InnovaSpace, All Rights Reserved


 RSS Feed
RSS Feed